Recognizing Hypothermia, Frostbite And Other Common Cold-related Illnesses – Toolbox Talks

Toolbox Talks are intended to facilitate worksite health and safety conversations. Click here to download talking points on recognizing cold-related illnesses to share with your crew.
Weather patterns are changing. Seasons becoming more extreme. And the ever-increasing unpredictability of Mother Nature is making it harder than ever for workers exposed to her wild weather swings to prepare.
Take the winter of 2013-14, for example. That’s when a polar vortex settled on top of much of the U.S., helping push that February into the record books as the coldest month in the history of weather observations. Much of the Midwest and East Coast were paralyzed by the cold. The moderately warm fall preceding it only exacerbated matters, with the quick turn in temperatures leaving people less ready to handle winter’s arctic shock.
With these cold-weather extremes as a backdrop, it’s more important than ever to be able to properly identify the most common cold-related illnesses, along with knowing what treatments to seek.
HOW THE BODY REACTS TO COLD
- Energy is spent maintaining internal temperature
- Blood is drawn away from extremities to the core
- Exposed skin & extremities cool rapidly, increasing risk of frostbite and hypothermia
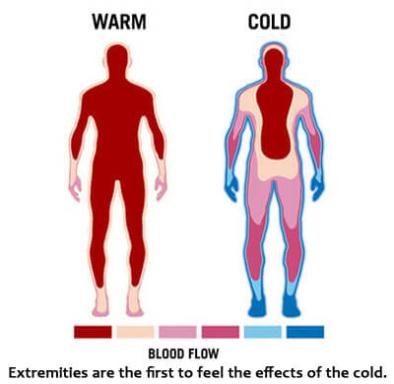
When the body temperature drops below 98.6 degrees Fahrenheit (or 37 degrees Celsius), blood begins to flow away from the extremities to heat the body’s core. This immediately cools exposed skin and extremities, and increases the risk of cold stress, specifically frostbite and hypothermia. According to the Centers for Disease Control and Prevention (CDC), early signs and symptoms of heat loss include shivering, fatigue and confusion or disorientation. They can evolve to include blue skin, a slow pulse, and even loss of consciousness.
If body temps continue to fall, dexterity is diminished and speech may be slurred. At 85°F (29.4°C), severe hypothermia – a condition characterized by an extreme low body temperature – sets in. Symptoms include cool skin, severe shaking and memory lapses, among other issues. Once the body temperature plummets below 78°F (25.5°C), a person is at risk for brain damage – and even death – if not treated immediately.
COMMON COLD-RELATED ILLNESSES
- Hypothermia
- Frostbite
- Trench foot
- Indoor and outdoor workers at risk

The three most common cold-related illnesses – hypothermia, frostbite and trench foot – are an obvious danger for those working outdoors in unpredictable winter weather. But the risk for those working indoors in places such as food processing, cold storage and beverage/brewing facilities is just as real.
Hypothermia
The most severe of the cold-related illnesses occurs when body heat is lost faster than what’s produced, and core body temp drops below 95°F (35°C).
What to look for:
- Shivering
- Poor coordination and slowing of pace
- Stumbling and clumsiness
- Dazed and confused behavior
- Slurred and slow speech
- Hallucinations or changes in personality
What to do:
- Mild Case: Move to warm area and stay active. Cover head and body with dry clothes or blankets. Drink a warm (not hot) drink.
- Moderate Case: Same as Mild, plus contact emergency medical personnel. Re-warm extremities.
- Severe Case: Treat worker very gently and do not apply external heat to re-warm. Hospital treatment is required.
Frostbite
Because of the way blood leaves the extremities to protect vital organs in the body’s core in cold environments, hands and feet are the most susceptible to frostbite.
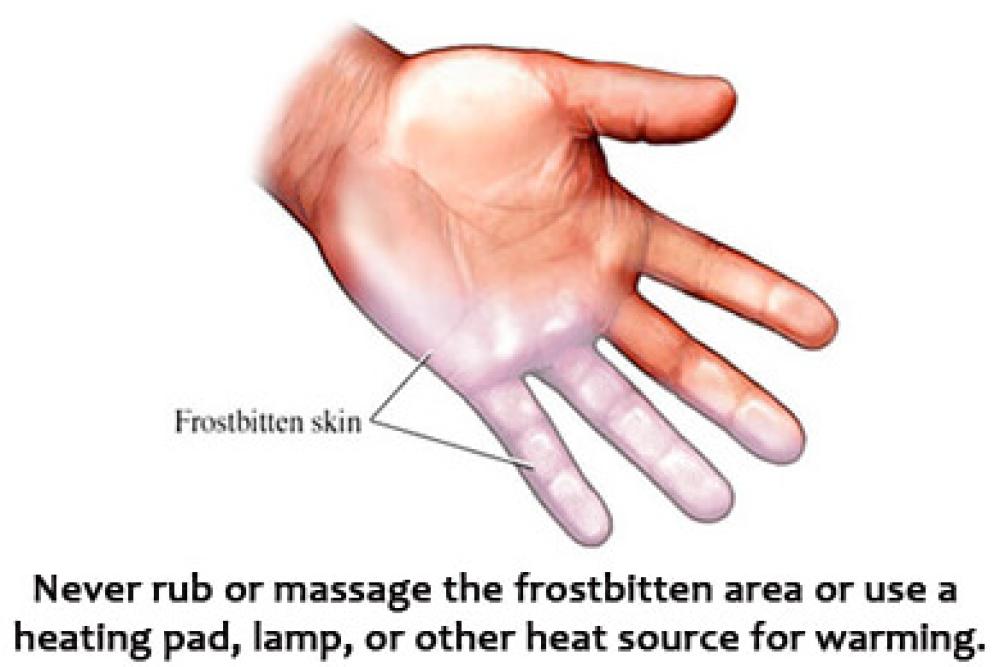
What to look for:
- White, grayish, or bluish skin
- Cold, hard, or waxy feel to skin
- May itch, burn, or feel numb
- Blistering and hardening of skin are signs of extreme frostbite
What to do:
- Get out of the cold
- Gradually warm the affected skin
- Place frostbitten areas in warm – not hot – water
- Wrap affected areas in a warm blanket
- Seek emergency medical help ASAP
NOTE: Do not rub or massage the frostbitten area or use a heating pad, heat lamp or other heat source for warming.
Trench foot
Trench foot is a “wet cold disease” occurring in damp or wet environments that are just above freezing. The name comes from WWI when soldiers developed the illness while waiting in the trenches for combat. The skin does not actually freeze with trench foot, but other issues definitely can arise.

What to look for:
- Numbness
- Swelling
- Blisters
What to do:
- Remove wet socks and footwear
- Thoroughly clean with warm water
- Dry feet
- When sleeping or resting, do not wear socks
- Get medical treatment ASAP
PERSONAL RISK FACTORS
- Age, weight, fitness level
- Chronic or acute illness
- Alcohol or drugs
- Acclimatization
- Dehydration

There are two sets of factors that come into play when considering the causes of cold stress on the body: personal and environmental. Being aware of these factors and knowing an individual’s risk factors will allow that person to be better prepared when the cold weather hits. While workers can’t do anything about some personal risk factors (like age, for example. The very young and the very old are much more susceptible to cold temps), they can reduce risk by being mindful of their own fitness levels -- watching their weight, staying hydrated, avoiding alcohol and drugs, getting plenty of sleep, etc.
Additionally, acclimatization -- gradually increasing exposure to the cold -- plays a large part in reducing stress on the body. By taking frequent warming breaks and avoiding the temptation to go “all in”, workers can build up tolerance to frigid temps.
ENVIRONMENTAL FACTORS
- Cold air temperatures
- High wind speeds
- Damp air
- Contact with cold water or surfaces
- Working without proper PPE

Four environmental factors contribute to cold stress: cold air temperatures, high velocity air movement, dampness of the air, and contact with cold water or surfaces. A cold environment forces the body to work harder to maintain its temperature. Cold ambient air temperature, water, and snow all draw heat from the body. High wind speeds and dampness in the air will also accelerate a body’s heat loss.
TALK TO YOUR CREW
The reality is that work doesn’t stop when the temperature drops. So taking a few minutes before a shift to educate your crew on the signs, symptoms and causes of cold-related illnesses is a simple yet effective measure to increase awareness and reduce the risks.


